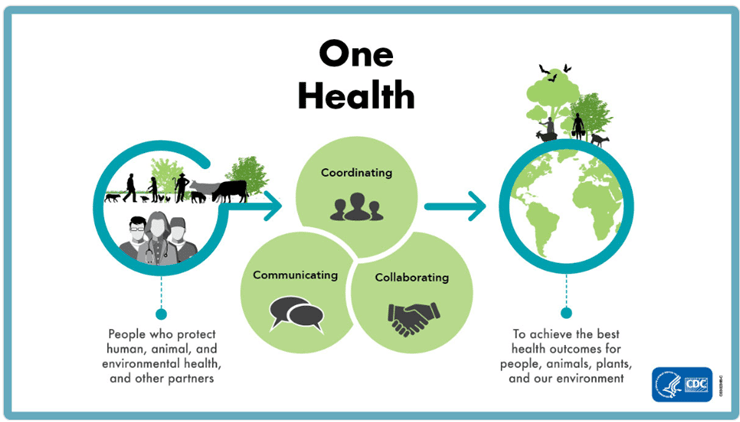
One Health is a collaborative, transdisciplinary approach that promotes optimal health by recognizing the interconnectedness of people, animals (both domestic and wildlife), plants, and the environment we share. Its importance has grown in recent years as interactions among these systems have evolved, intensifying human–animal–environment interfaces. Factors such as demographic expansion, land use changes, and increased international movement have contributed to these shifts, creating more opportunities for zoonotic disease transmission and underscoring the need for coordinated surveillance, prevention, and response efforts (CDC - One Health).
Zoonotic diseases, which spread between animals and people, are extremely common worldwide. People can experience anything from mild to severe illness from zoonotic diseases, sometimes even when the animals carrying the germs seem completely healthy. It is estimated that 60% of all infectious diseases are zoonotic and 75% of all emerging infectious diseases in people come from animals (CDC - Zoonotic Diseases). Who are the One Health players? One Health brings together experts from multiple sectors to better prevent, detect, and respond to health threats—especially zoonotic diseases that move between animals and people. No single discipline can address these issues alone, so effective public health action depends on strong communication, coordination, and collaboration across disciplines and sectors (CDC - One Health). Key One Health partners and their roles: • Human Health Professionals – Doctors, nurses, epidemiologists, laboratory scientists, and public health practitioners monitor human illness trends, investigate outbreaks, diagnose disease, and guide prevention strategies. • Animal Health Professionals – Veterinarians, veterinary technician, laboratory scientists, and agricultural workers identify disease in domestic and wild animals, track animal outbreaks, improve animal care, and reduce risks of disease transmission from animals to people. • Environmental Health Experts – Ecologists, environmental scientists, wildlife biologists, and conservation specialists study environmental changes, habitats, water quality, climate impacts, and how these factors influence disease spread among animals, humans, and plants. • Other Relevant Players – Farmers, policymakers, pet owners, law enforcement, educators, and communities contribute expertise in areas like biosecurity, education, land use, and emergency planning. What are some notable One Health issues relevant for virologists? • Antimicrobial Resistance – Pathogens that are resistant to antimicrobial agents and drugs can circulate in communities, food systems, healthcare settings, and the environment and make people and animals sick. Antiviral resistance is most common when used to treat viral infections for an extended amount of time. Examples include HIV, hepatitis B (HBV) and C virus (HCV), and herpesviruses (Cleveland Clinic Antiviral-Resistance). • Vector-Borne Diseases – Mosquito and tick habitats have expanded through climate change, globalization, and urbanization, which in turn contributes to the spread of vector-borne diseases (WHO - Vector-Borne Diseases). A key example is West Nile virus (WNV), which emerged in the US in 1999 and is frequently transmitted between birds and mosquitoes with humans and horses often serving as incidental hosts. WNV is now the most commonly reported domestic arboviral (arthropod-borne) disease accounting for ~95% of all reported cases (WNV - MMWR). Another example of increasing importance in recent years is dengue virus (DENV). DENV incidence has been increasing exponentially because there are more mosquitoes in more places, more people traveling, and because of its cyclical nature (CDC - Dengue Facts). • Food Animal Diseases – Illnesses in food animals can disrupt food supplies, livelihoods, and economies. Viral infections such as Highly Pathogenic Avian Influenza (HPAI), African swine fever (ASF), and foot and mouth disease (FMD) have and continue to cause massive economic loss globally. FMD and ASF are not zoonotic, but economic losses range from $6.5-21 billion annually for FMD (WOAH - Foot and mouth disease), and the economic loss for the 2018-2019 ASF outbreak in China exceeded $200 billion (WOAH - African swine fever). • Waterborne Diseases – Contaminated drinking, recreation, or other water sources can make people and animals sick. Domestically, about 1 in 5 waterborne diseases are caused by norovirus (EID - Waterborne Disease). Worldwide, other viruses such as hepatitis A virus have a higher disease burden with over 100 million infections reported annually (Global hepatitis report 2024). • Zoonotic Diseases – Zoonotic diseases are spread when humans have close proximity to animals (wildlife, agricultural animals, and pets). Some examples of key zoonotic viruses not mentioned above are rabies virus, Ebola virus, and SARS-CoV-2. Rabies is preventable but nearly 100% fatal if not treated before symptoms appear. In the US, less than 10 human cases are reported annually and over 90% of animal rabies cases are reported in wildlife such as bats and raccoons. Worldwide, 95% of the ~70,000 human rabies cases reported annually originate from domestic dogs (CDC - Rabies). • Noncommunicable Diseases – Noncommunicable diseases accounted for ~75% of non-pandemic-relate deaths in 2021, and the four main types are cardiovascular disease, cancer, chronic respiratory disease, and diabetes (WHO - Noncommunicable diseases). Although noncommunicable diseases are not transmissible, viral infections can act as triggers for or exacerbate these chronic conditions. For example, viruses such as human papillomavirus (HPV) and Epstein-Barr virus (EBV) are known to cause cancer.
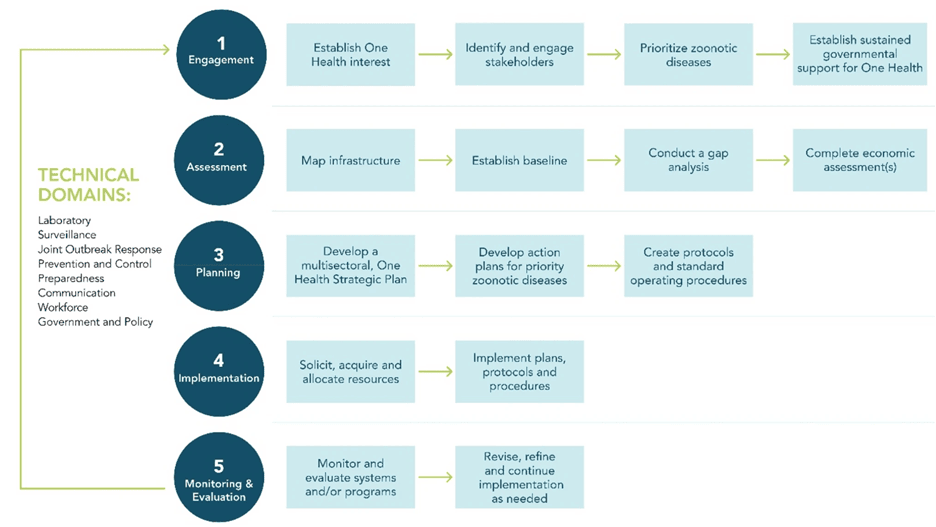
How are One Health players working together to combat the spread of zoonotic viruses? Internationally, the Tripartite organizations (Food and Agriculture Organization (FAO), World Organisation for Animal Health (WOAH), and World Health Organization (WHO) are utilizing a multisectoral, One Health approach to address zoonotic diseases in countries through mandated inter-agency collaboration and the establishment of a guide (Tripartite Zoonoses Guide) to facilitate sustained collaboration at the local, subnational, national, regional, and international level. In the United States, the CDC, FAO, and other subject matter experts have developed a Generalized One Health Framework (GOHF) which is based upon the Tripartite Zoonoses Guide approach and aims to provide recommendations to improve multisectoral collaboration and enhance zoonotic disease prevention and control. This framework includes 5 key steps: engagement, assessment, planning, implementation, monitoring and evaluation.
Timely, accurate, and reliable diagnostic testing is essential for any effective zoonotic disease control program, yet human health, veterinary, and environmental laboratories often work in parallel without aligning methods or sharing data—leading to inefficiencies and duplicated effort. A multisectoral One Health laboratory approach can reduce costs and accelerate outbreak detection by coordinating infrastructure, standardizing protocols, and sharing samples, personnel, equipment, and data where appropriate. Here are a couple real world examples of One Health in action: • In Canada, co-located high-containment laboratories for human and animal pathogens support integrated, cross-cutting research on high-consequence zoonotic pathogens such as Zika and Ebola viruses. Even when labs operate independently, aligning procedures and exchanging standardized data enables faster identification of outbreaks and sources of infection. • PulseNet—a coordinated network of food, animal, and public health laboratories—illustrates successful laboratory data sharing, having prevented an estimated 270,000 foodborne illnesses and saved hundreds of millions of dollars annually through shared laboratory-based surveillance. How can laboratory scientists lead the way in One Health? As the frontline stewards of pathogen detection, characterization, and data integrity, laboratory scientists, including virologists, are uniquely positioned to drive the success of the One Health approach. Zoonotic threats do not respect the boundaries between human, animal, and environmental systems—and neither can our laboratory practices. When laboratory networks work in isolation, we risk delayed detection, duplicated efforts, and missed opportunities to prevent or mitigate outbreaks before they escalate. Virologists can use their expertise and scientific insight to bridge these gaps. By aligning methods across sectors, harmonizing diagnostic protocols, and sharing data in real time, laboratory professionals can accelerate outbreak detection, reveal transmission pathways, and strengthen preparedness at every scale. When laboratories collaborate across disciplines, they expand capacity and protect public health more effectively. So how can virologists help to shift the mindset and pave the way for One Health? Seek out your counterparts in human, animal, and environmental academic, industrial, and government laboratories. Connect by attending conferences and seminars, participating in workshops and training courses, being present on academic social media platforms and online forums (colLABorate - Association of Public Health Laboratories), joining professional organizations such as ASV, serving on committees, boards, and review panels, and applying for grants that require a more transdisciplinary approach. Work toward establishing shared protocols, participating in multisectoral surveillance, advocate for integrated data systems, and championing a culture where collaboration replaces silos. By adopting and advancing the One Health approach, laboratorians can help transform how communities, nations, and global systems detect and respond to zoonotic threats. |